Trick Question: What’s the Answer to Drug Abuse?
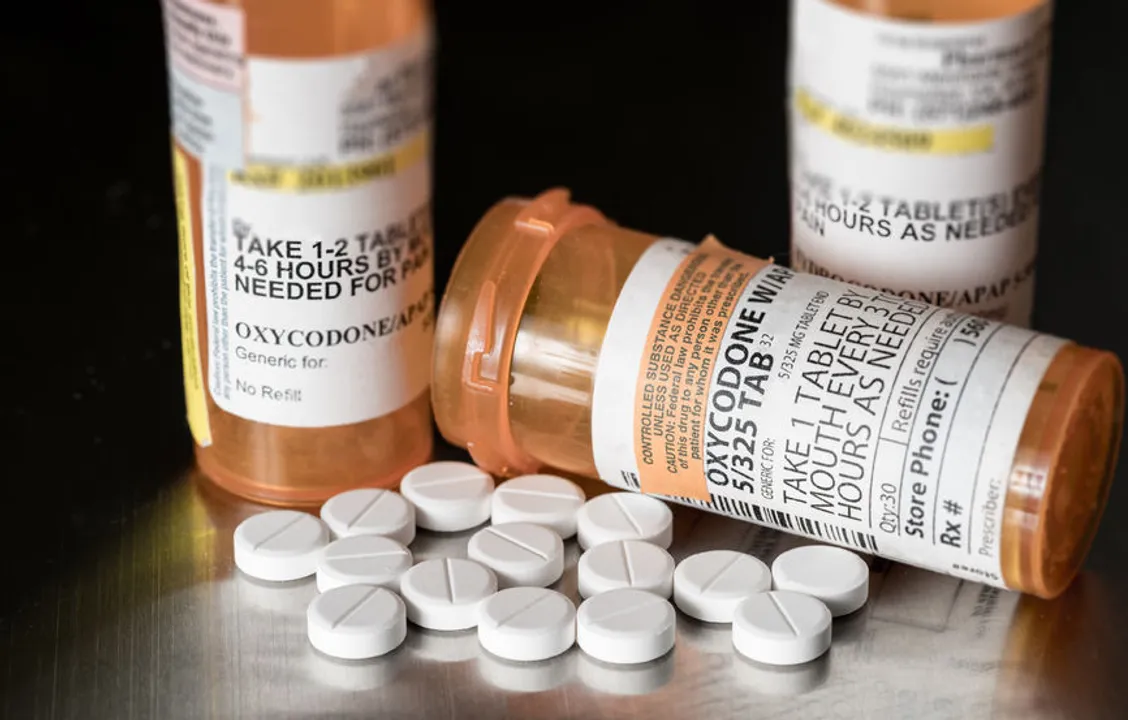
Steven Heap/123RF.com
“...life without Pain is a long endless chain
Of errors repeated again and again
So don’t be afraid of Pain don’t run away...”
--Pose Ode, by Pain
Ouch!
Pain is a warning signal. It’s the message from the environment that goes straight to the brain and tells it, “Don’t do that. It’s bad.” From touching a hot stove to teasing a large, sharp-toothed feral carnivore, we learn, and for those of us who may not get it, we even have an invisible brain telling us not to do things--reflexes. Reflexes are why we jump from a damaging stimulus before we even start to hurt from it, why we blink at the bug in our eye before we even see it. Our species depends on pain and even those reflexes that by-pass the thinking brain.
So we hurt. We cry, yelp, and jump away. And then an even more amazing thing happens. What if we’re so injured we cannot jump away from that large toothy mauler? The brain, in its wisdom, relies on a tiny chunk of neural real estate called the locus ceruleus (LC), which makes a neurotransmitter called norepinephrine. Among the LC’s many functions, it sends down a pain-lessening signal so that we can jump away from our nemesis, even when logic says we shouldn’t be able to do this. (It’s why when you hit your thumb and grab it, it doesn’t hurt so much a moment later--it’s not because your thumb is any less injured!)
You reap what you sow
From thousands of years ago to now, we harvested the opium poppy and eventually the morphine molecule to give the LC some competition. The LC tones down the pain signals initiated by injury, but narcotics, when they fill the opioid receptor site's on neurons, block the pain signals from registering at the brain level, and the LC's response doesn't even happen. The problem is, it’s hard to get one thing to do only one thing, when most things in the body do hundreds of things. So with the pain relief of narcotics comes euphoria, dependence, tolerance, and addiction.
Of mice and men
Life tends to seek rewards via the path of least resistance. Mice that have implanted electrodes to stimulate their pleasure centers will tap the little firing lever repeatedly, incessantly, until they die of starvation.
These are not bad mice. Like the people in crack houses who die before they know it, teenagers take prescription drugs for other than legitimate medical purposes, go to sleep, and then don’t wake up. This is the collateral damage of making drugs that relieve pain.
Two types of pain
The brain’s LC can be defeated. Repeated episodes of acute pain make it ineffective when the acute pain processes become overwhelmed, turning on another type of pain receptor--one that puts out continued pain even when the original site of injury is healed. That’s when acute pain becomes chronic pain, and it’s when a second edge of the opioid sword begins to cut. When chronic pain self-perpetuates, you can numb it with narcotics, but you cannot turn it off with narcotics. This means that if you use narcotics for chronic pain now, you’ll be using it 5 years from now, but more of it. Tolerance means you need more to get the same effect as time goes on. It gets worse: dependence means you suffer without it; and addiction means you would do anything--even break the law--to keep the stuff coming.
It gets even worse: while acute pain provokes anger (again, think hammer-to-the-thumb), chronic pain creates depression, and both depression and pain potentiate each other in a downward spiral that creates a perfect storm of debilitation on both the physical and mental fronts.
The answer
If prescription drugs cause a problem, many reason, clamp controls on them. Make it harder to get them. Threaten those who get them illegally with felonies. Imprison addicts. What this ignores is the same thing that kills the mice tapping their pleasure levers. Addiction is a rewiring of the brain, and victims are driven to make poor choices. Drugs make smart people dumb and turn good people bad, but only about 15% of them. The rest can dabble in narcotics and never develop this problem. For those 15%, though, genetics plays the Tarot card of doom.
For the record, it’s a mental health problem, and there’s very little mental health in the prisons.
The biggest cause of chronic pain is inadequately treated acute pain--that pain in which opioids benefit people the most. A broken arm, a kidney stone, even a heart attack--yes, they’re helpful in acute pain. When we use them for chronic pain, however, we’re just kidding ourselves.
The problem: kidding ourselves notwithstanding, when behavioral modification, physical therapy, yoga, and even acupuncture fail in relieving chronic pain, the only thing left is the narcotic.
The answer: there is no answer.
Legislating the brain
More people now die from opioid overdoses than from car accidents. These are the children of mothers and fathers. These are husbands, wives, and other loved ones. People notice. People complain. People gather, demanding action. Politicians and law enforcement are seduced by the idea that if the source is controlled, the problem will be solved, but that ignores the 15% of those genetically predisposed to addiction. Prescription drug use goes up, heroin use goes down; crack down on prescription drugs, heroin deaths begin to rise again. And so it goes.
Clamping down sounds like a good idea, but those 15% will succumb to pitfalls of the next addiction du jour. Meanwhile, the folks that rely on narcotics--a poor second choice until something better comes--have their already-difficult lives made even harder. Rules such as no more than 3 days prescribed at a time and scrutiny that dissuades pharmacies from even carrying narcotics makes legitimate users scramble every 3 days to find a pharmacy that’ll fill their prescriptions.
In pain? We don’t care. Drop dead.
This is the mantra of the government. No one notices when someone with rheumatoid arthritis has a tough time getting relief. But an opioid overdose is hard to miss, and it’s even harder to accept. Even outside of the genetics, good kids do stupid things sometimes and end up dead. And while opioids for chronic pain really don’t work in the long term, try explaining that to the guy whose spine is held together with at titanium cage who needs to be on that roof tomorrow firing a nail gun or he won’t get paid. It seems that many of the people who need it to function are often a paycheck away from a shelter.
Until we develop drugs for severe, chronic pain that are effective, cheap, non-addictive, and don’t develop tolerance, we’re stuck with the crap that’s out there.
Related Posts
